The metro-east has some of Illinois' worst nursing homes, data says. Here's why.
In 2015, Ellen Paule, 79, of Belleville was admitted to St. Paul’s Nursing Home in Belleville. Within two months, a wound on her heel deteriorated to the point that live larvae and maggots were found crawling inside it.
Paule was hospitalized on June 28 with “a wound infection and maggot infestation,” according to reports from the federal Centers for Medicare and Medicaid. Another resident reported that the dressing on Paule’s leg ulcer would at times go two or three days without being changed.
CMS blamed the nursing home staff for the neglect of Paule and issued the home a severe violation.
Paule died two years laterin April 2017. Efforts to reach her family for comment were unsuccessful.
At Belleville's Midwest Respiratory and Rehab, a diabetic resident fell into a “permanent vegetative state” in 2015 when staff failed to give her insulin for two weeks, according to reports from the Illinois Department of Public Health.
The facility, which is owned by Integrity Healthcare, was fined $25,000 and issued a severe violation by IDPH.
St. Paul’s executive director, Tammy von Yeast, said via email she could not comment on Paule's case because she is prohibited from providing information regarding residents' care and treatment.
An Integrity Healthcare representative also said she could not comment on specific cases due to privacy laws.
The citations issued to St. Paul and Midwest Respiratory and Rehab are just a few of hundreds issued to metro-east nursing homes in the past three years. It and many other local nursing homes have been issued violations at a rate that far exceeds state and federal levels.
Nursing homes across the state, and especially in the metro-east, appear to be struggling to provide quality care. Critics say this is possibly due to inadequate government reimbursement or perhaps a failure to invest enough in staffing and patient care.
Local facilities have been issued numerous violations for neglect, bedsores, failure to investigate residents’ injuries and other issues.
Some blame nursing home owners for the lack of proper care in these homes, claiming corporations and owners are funneling money away from staffing and residents’ care and into their own pockets.
Others, however, blame Illinois’ privatized Medicare and Medicaid system, from which medical reimbursements arrive months late and are often too low to cover costs. Facility representatives say a backlog in reimbursements from Managed Care Organizations, health insurance corporations who control Illinois Medicare payments, are causing a crisis for facilities.
Whatever the cause, state and federal data shows metro-east nursing homes are facing a problem with violations issued on the state and federal level.
▪ Six residents died due to improper care in metro-east nursing homes from 2015-17, according to the Illinois Department of Public Health. Two more residents were sent into permanent comas because of nursing home errors, the department said.
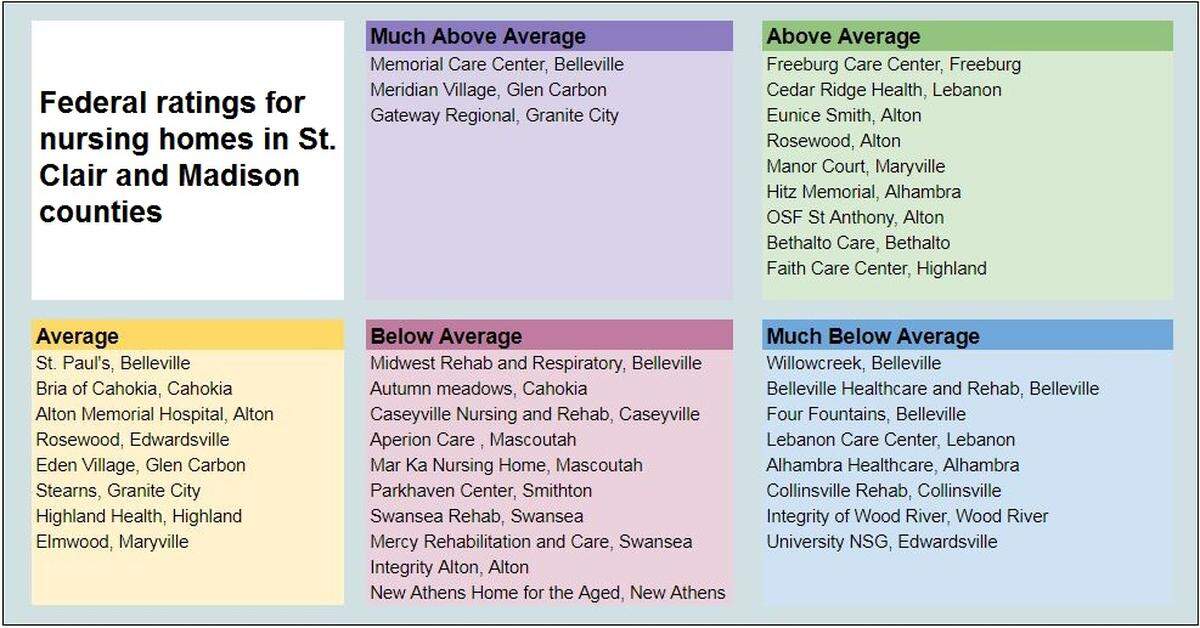
▪ Thirteen out of St. Clair County’s 18 nursing homes score “below average” in overall care, including Midwest Rehab, according to the Centers for Medicare and Medicaid Services. Four of those have a rating of "much below average."
▪ In the past three inspection cycles, five of Belleville’s nursing homes have received a total of 260 federal violations, for an average of 17.3 health violations per home each inspection. This is more than double the state average of 6.2 per inspectionand more than triple the national average of 5.8, according to the Centers for Medicare and Medicaid Services.
Columbia-based lawyer Steve Buser, who has worked in the metro-east for 40 years, said each year he works on 10 to 15 cases alleging nursing home neglect, abuse or improper deaths. However, he noted he receives requests for about 10 times that amount.
“I keep getting calls, usually several a month at least, and I probably only take one out of 20 cases,” Buser said. “My phone doesn't quit ringing.”
A pattern of neglect
Buser serves clients throughout Missouri and Illinois, but said most of his nursing home cases come from St. Clair and Madison counties.
Nursing homes can receive violations on the state and federal level and are inspected at least once every six to 15 months.
Federal inspections, organized by CMS, issue 12 levels of violations. The level depends on the amount of harm caused and the number of people potentially or actually harmed.
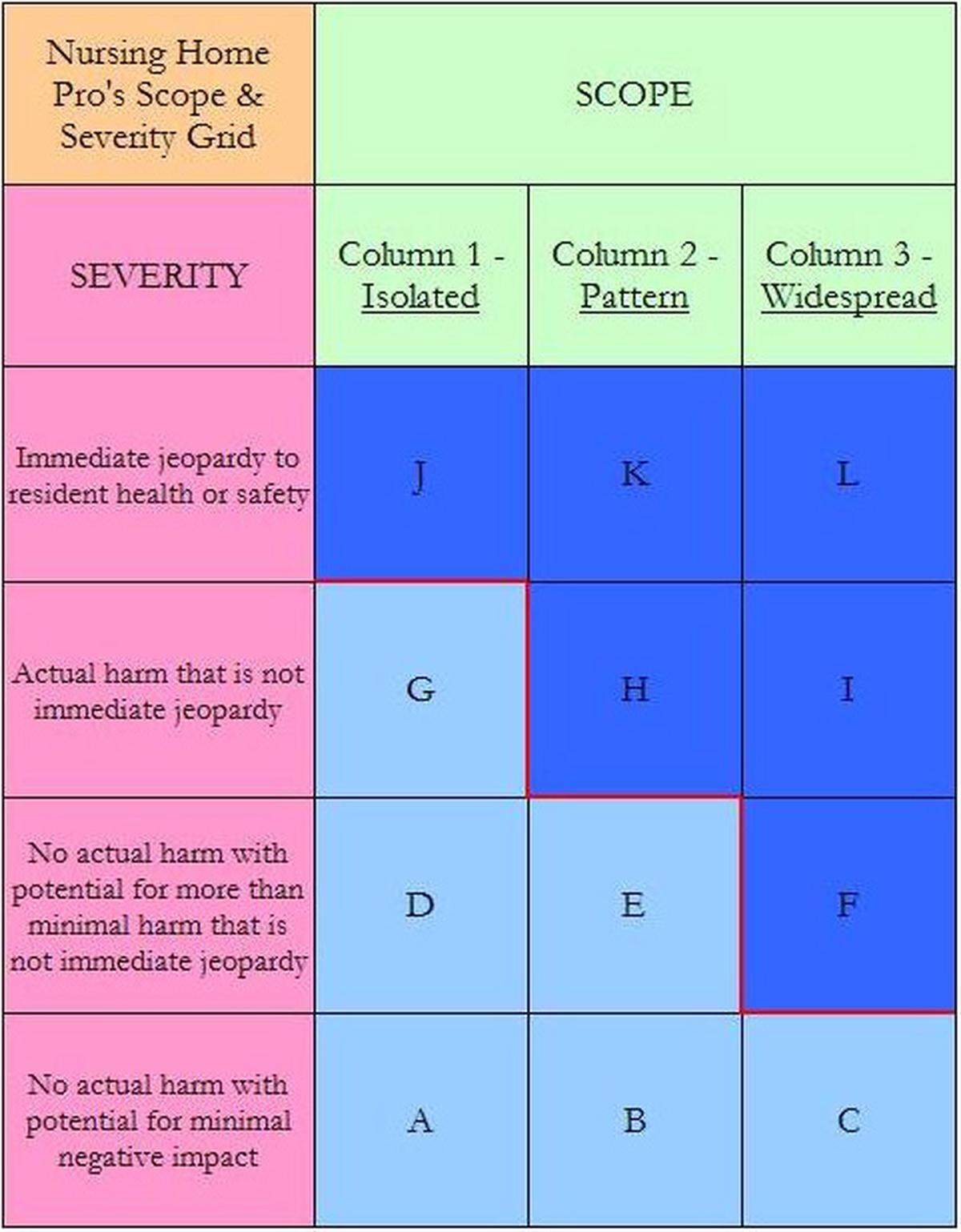
An “A” violation, for example, means there was the potential for minimal harm for a very small number of people. An “L” violation, the most severe a home can receive, means there was widespread, immediate jeopardy to residents’ health or safety.
The Illinois Department of Public Health also issues violations to homes based on CMS inspections and range in severity.
Since November 2014, only 28 L violations have been given by the state. Eight of those violations, 28.6 percent overall, were given to metro-east nursing homes. Seven were issued in St. Clair County alone, according to CMS.
When a violation is issued, an agency can fine the home up to $25,000 per offense depending on its severity. CMS can revoke a home’s Medicare and Medicaid reimbursement if they see fit.
Some violations, such as four issued against Cahokia’s Autumn Meadows, were based around a specific incident. In July 2016, the home received multiple “L” violations when a fire broke out in the home. IDPH claims staff did not have an adequate emergency plan in place for patients. Autumn Meadows representatives disagree and say they are appealing the violations.
Other severe violations in the area indicate a pattern of neglect and endangerment of patients.
For example, Integrity Healthcare in Wood River was issued a violation after a patient was sent to the hospital in a coma on Christmas with a 104.1 degree fever and sepsis. The man had been unresponsive for five days prior to his hospitalization, according to the report, and the facility had failed to “recognize, assess and treat” the man’s condition.
Data shows many homes are not issued a violation just once, but instead are repeatedly given citations for the same problems over and over again.
All deficiency data used in this story is based on 2015 to 2017 CMS reports available as of April 1, 2018.
At Cahokia’s Autumn Meadows, 9 of the 13 violations issued in 2017 were repeat violations, such as keeping residents free from physical restraints.
Jeff Davis, the director of operations of Southwest Healthcare Management, which owns Autumn Meadows, said repeat violations do not necessarily indicate the exact problem is recurring. In some cases, he said, a new violation may differ from a previous one but still fall under the same code because the categories are so broad.
“We may have corrected part of the problem but not all the aspects of it,” he said. “We have systems designed to prevent any violations that we have here, and sometimes those things need to be improved upon and they’re called out by state violations. We always take steps to re-mediate those.”
Integrity Healthcare in Belleville was issued four citations in two years for not providing care that ensured the highest well-being of each resident. Within an overlapping 15-month period, the facility was cited four times for not preventing avoidable accidents or protecting against accident hazards.
One of these violations in 2015 resulted in the hospitalization and severe injury of a resident whose tracheostomy tube was ripped out because he was moved improperly.
Helia Healthcare, which owns Willowcreek and Four Fountains in Belleville, was cited six times in two years for failing to prevent and treat bed and pressure sores; once in 2015, four times in 2016 and once in 2017.
Bedsores are one of the of the most common, and painful, issues in nursing homes.
Bedsores, or pressure ulcers, are caused when people remain in one position for too long. This puts pressure on the skin, opening up sores and leading to infection, sepsis and even death if left untreated.
Ellen Paule's maggot infestation, for example, was due to the dressing on her ulcer not being changed often enough, according to the violation issued by the Illinois Department of Health. The home was fined $2,200.
“With good nursing care, this could have been avoided,” Paule’s doctor said in the report.
Since 2014, St. Paul’s has been issued three more violations for not preventing or treating bed sores properly.
Paule filed a lawsuit against the home in March 2017. She died in April 2017 and the case was dismissed.
Repeated violations
In January 2012, Aubrey Giles, 77, who suffered from dementia, wandered away from Midwest Rehab and Respiratory Center, according to IDPH reports. His body was found in a nearby creek bed the morning after he was reported missing; he had died of hypothermia.
The facility, owned by Integrity Healthcare, was fined $55,000 for Giles' death.
In 2016, the facility received a violation for the same issue — not ensuring the home was free from accident hazards and not providing supervision to prevent them. The next month, they were again issued a more severe violation for the same thing.
Additionally, in March 2015, Juanita Cleda Simmons was left unsupervised at Midwest Rehab as she wandered down a hallway in her wheelchair, which she was illegally restrained into, and opened a fire exit door leading to a stairwell, according to Illinois Department of Health reports. The door’s alarm had been lowered to a chime instead of an alarm for unknown reasons. Simmons fell down the staircase and died.
IDPH imposed a $50,000 fine on the home for Simmon’s death, saying they failed to prevent the accident.
Brad Badgley, a Belleville lawyer, handled Simmons' case on behalf of her daughter, Mary Roth.
“It’s a sad area. The people involved are in the most vulnerable points in their lives,” Badgley said.
In December 2016, Simmons’ family received an undisclosed amount of money in a wrongful death settlement with the home.
Even after Giles’ and Simmons’ death, Integrity received yet another violation for not preventing avoidable accidents in September 2016 when an unsecured ramp leading onto a van caused a resident to fall from his wheelchair. Another resident fell and hit his head while being moved by staff.
“The bottom line is the nursing homes have an obligation to maintain a certain standard of care, and they seem to have a difficult time doing that,” Badgley said. “As a result, you have people in unfortunate circumstances either get injured or die.”
Caught in the middle
Davis, of SW Healthcare, said facilities, including his own at Autumn Meadows and Caseyville Rehab, have become increasingly limited in resources under Illinois’ Managed Care Organizations, also known as Health Maintenance Organizations.
Those two facilities alone are currently owed more than half-a-million dollars by the state for care they already provided.
Pat Comstock, executive director of Health Care Council of Illinois, said nursing homes in the state are facing increasing systemic challenges.
“Our facilities and nursing homes in general are home to the most vulnerable populations in health care,” she said. “At the same time, the rates the state pays for Medicaid recipients has been historically very low, and Illinois is lower than its surrounding states.”
Long-term care facilities in Illinois are increasingly underfunded and losing money as the state consistently fails to reimburse them for medical care, according to facility representatives.
About three years ago, Illinois began shifting Medicaid and Medicare payment responsibilities to corporate networks of private insurers called Health Maintenance Organizations.
Previously, the Department of Healthcare and Family Services controlled payment. Now, HMO’s are paid by the department and are responsible for reimbursing nursing homes for the care they provide.
Comstock said facilities might wait up to 10 months to receive payment for medical care they provided. When payments do go through, they are often at very low rates and don’t cover the cost of care.
“The state of Illinois has failed to be a good partner in providing care,” Comstock said. “At the same time, there are regulations demanded of us, we don’t have a good partner on the payment side to ensure that we have the sources we need to meet those obligations.”
Comstock said this has created an environment where facilities never know when the next check is coming, or if it will be enough to cover the cost of care. To pay for resident care, facilities have to take out private loans. In some cases, Comstock said, facility owners have mortgaged their own houses to pay for care.
.png)
Davis said at Autumn Meadows and Caseyville Rehab, they have 31 patients out of about 200 whose Medicaid payments are still pending. Along with pending patients still in the facilities, 64 patients were discharged before their Medicaid applications were complete.
This means the facilities are waiting on payments for 95 former or current residents. Between both facilities, the state owes about $726,000 to Autumn Meadows and Caseyville Rehab for these residents’ care.
If any of those pending applications are denied, the facilities are simply out the cost for care.
Davis said these challenges make finding resources for facilities increasingly difficult. He said they’ve paid for residents’ doctor appointments, dentures, hearing aids and ancillary services out of pocket.
“We’re resource limited, but our residents come first. With any Medicaid pendings, we end up having to pay that service so that residents get that care they need,” he said. “There’s no way we can go back and bill Medicaid in some cases.”
Davis thinks Illinois Department of Family Services might have shifted to HMOs as a cost-saving measure.
“My perception is that as a stakeholder in this process, that we maybe weren’t considered.” he said.
Comstock said the issue with Medicaid payments have left facilities in an impossible position.
“We are caught in the middle between a system that wants to look for every reason not to pay us and the care we know our residents need,” she said.
The staffing problem
Margy Pearson placed her mother, Ruth Waldron, in St. Paul’s home in Belleville in June 2015. Almost immediately, she was concerned about her mother’s care. At one point, she said her mother went 12 days without a shower, causing her to develop a urinary tract infection.
"It just makes us sick that she had to live out her last days like that," she said.
In emails provided by Pearson between herself and Mindy Hanna, director of nursing at St. Paul’s at the time, Pearson told Hanna she was concerned about her mother’s health because she was “very susceptible to bladder infections.”
“If mom hasn’t received a shower, then I believe no one else has as well. This to me, is a very serious health hazard for senior citizens,” she wrote in an email on Aug. 19, 2015 . “We have put her in the care of St. Paul’s Home to give her round the clock care that she so needs. This is very disappointing.”
Pearson said the day she emailed Hanna, her mom finally got to take a shower.
“Please know I am working really hard with staff trying to educate them and help them understand the importance of every aspect of care,” Hanna wrote in a reply to Pearson. “I do realize there are some issues here that need to be resolved."
Many, such as Pearson, believe problems like the ones she faced are caused by a misallocation of money on the part of the nursing home company. Low funding can mean homes are understaffed and staff are under-trained.
Based on 40 years of legal experience with nursing homes, Buser, the lawyer who handles nursing home cases, agreed.
“They tend to put profits before people. It sounds like a trite phrase, but that’s where the real problem is as opposed to someone saying that accidents just happen,” said Buser, who has worked in the metro-east for 40 years.
At St. Paul’s, general services (diet, food, housekeeping, etc.) costs have increased by 8.5 percent from 2006 to 2016. Administrative costs (administrative salaries, professional services, etc.) increased by 136 percent, according to cost reports filed with the state.
Kimberly Patterson has been working in senior care for 25 years. She has been the director and executive director at multiple homes, including the Shrine, Parkway Gardens in Fairview Heights and the Colonnade Senior Living and Heritage Community in O’Fallon.
Patterson said low wages for CNAs can contribute to a lack of thorough care.
“CNAs are the ones they are generally lower staffed in, they work very hard and not usually for a very good salary. You also see issues of even if they could have the staff for the patients they need, staff don't have the willingness, they don't want to do it, they don't have that person-centered care,” she said.
The following are the average hourly wages of CNAs at some of the area’s homes, according to reports filed with the state:
▪ Bria of Belleville: $11.76
▪ Integrity Belleville: $10.03
▪ Integrity Alton: $11.31
▪ Helia Southbelt: $12.99
▪ St. Paul’s: $12.39
▪ Cahokia Rehab: $11.79
Davis said they have been struggling with finding “caring, competent people in the right numbers” for staffing. Record unemployment lows have placed facilities in competition with places like McDonald’s, where workers can do less intense work for the same pay.
Davis also emphasized, however, their facilities are not understaffed.
“We go out of our way to make sure our residents have all that they need, but would I like to do more? Absolutely,” he said.
Patterson said she’s worked in both for-profit and nonprofit homes. She said in her experience, for-profit homes are more understaffed because the person who owns the home wants to get a return on their investment.
“I’ve worked for for-profits. They don't want to spend money on staff so that they can get a profit. They just want to have enough to get by,” she said. “They don't understand it because they're not on site. They’re willing to push staff, when [staff] say ‘we need more staff,’ they say ‘just deal with it.”
Davis, however, said he disagrees with the notion that corporations are pocketing money for themselves instead of caring for residents.
“Never once have I gone to my owners and said my residents need something and they’ve told me no,” he said.
“We’ve bought dentures, we’ve bought hearing aids, we’ve bought medications when Medicaid is not approving it or when there’s a delay. So I would challenge that perception through practical, real world happenings that have occurred in my experience with my company.”
Consequences of short staff
According to a study published by the Health Research and Educational Trust, high staffing levels, especially licensed staff, are associated with higher quality of care.
At St. Paul’s, the amount of time a registered nurse spends with each resident per day is much lower than the state average, with nurses spending an average of 10 minutes with residents versus the state average of 46 minutes.
CNA’s however, are above the state average at 2 hours and 22 minutes with each resident, while the state average is just more than 2 hours.
Buser, who focuses on nursing home cases, said understaffing causes large gaps in patient care, leading to these kind of incidents.
“Understaffing is one common factor in all of these cases,” Buser said. “It’s not the fault of the (CNAs), there are not enough of them and they are not trained properly. They are expected to do the work of people that are more qualified. They are expected to do work they cannot handle. There are other reasons too, but almost all the cases result from understaffing.”
Violation reports from CMS indicate understaffing causes neglect and mistreatment in nursing homes.
In 2015, Midwest Rehab and Respiratory in Bellevillereceived a severe violation when a patient’s tracheostomy tube was ripped out because he was moved improperly, according to CMS reports. The resident was taken to the emergency room and two weeks later was still unresponsive.
According to the CMS report, the man was moved onto a mechanical lift by one staff member instead of two, as policy requires. A resident who witnessed the event said the tube was pulled out while he was being transferred and “there was blood all over the place.”
According to the unnamed resident, workers regularly transfer patients by themselves because they don’t have enough staff. On the night of the incident, there were only three CNA’s for two floors of the home. There are supposed to be six total.
In March 2017, the facility, owned by Integrity Healthcare, received another violation because they did not have a registered nurse at the home every day. According to the report, there was no nurse at the home for at least two days in March, leaving 86 residents without a resident nurse.
Belleville resident Becky Eisele said when her mother was at St. Paul’s in 2015, she was constantly worried about her mother's quality of care.
"Mom always felt very unsafe," she said. ""I honestly could not wait to get my mom out of there."
Eisele said her mom had a wound on her leg that required routine treatment. Instead, Eisele said, the dressing would not get changed often enough.
“When I would come in and ask why, every time they would say they were just too short-staffed,” she said. “That is not an excuse for not doing my mom’s wound care.”
While medical records for Eisele's mother were not available, Eisele provide the BND with photos of her mother's wound while she was at St. Paul's.
St. Paul's declined to comment, citing state and federal privacy laws prohibitting the facility from providing information regarding resident care and treatment.
Eisele's mother was in St. Paul's at the same time Ellen Paule was when her wound became infected with maggots.
Eisele, who works at Barnes Hospital, said she was worried about her mother’s wound care since improper care can lead to infection and even death.
“If I wasn't on top of it, I guarantee it wouldn't have gotten changed as often as it should have,” she said.
Eisele did not file a formal complaint with St. Paul's.
‘No one should be treated like that’
Buser said money is spent “where the priority isn’t patient or resident care.”
Pearson said CNAs would refuse to take her mother to the bathroom, telling her she could only go “every two hours.” This often resulted in Waldron wetting her bed and lying laying there for hours.
In emails provided by Pearson, she told St. Paul's director that CNAs were telling her mother "they are trying to 'train' her bladder," causing "stress and anxiety for mom and hard feelings against the staff."
“She said a nurse came in one day and said we’re not going to do that, we’re going to retrain your bladder so you can only go every two hours,” Pearson said. “And she just looked so down when I came in that day. So I told them, you’re not going to retrain an 89-year-old woman’s bladder. It was like a huge ordeal for them to take her to the bathroom. She would ring the bell over and over and no one would come. No one should be treated like that.”
Pearson emphasized that she does not blame all of the staff for the issues she had with St. Paul’s.
“Don’t get me wrong, there are a lot of good employees there, some of the nurses we just adored. It’s just mostly the CNAs and people in the food service. They just don’t care. It was really sad,” she said.
Pearson said she thinks the hiring process and training should be more thorough to make sure people understand they’re responsible for people’s lives.
“I think if they had more training of what’s expected of them, things would be different,” she said. “Don’t take the job if you can’t do this. Because it’s not for wimps. “
When staff are not trained adequately, the consequences can be deadly.
Helia Healthcare received an L violation in March or April of 2016, which stated a resident died after staff failed to do CPR because they were incorrectly told the resident was under a “Do Not Resuscitate” order.
The resident actually was “full code,” meaning they previously indicated they wanted everything done to save them if their heart stopped beating, but a staff member did not receive proper training on the codes and looked at the wrong information. The staff member was fired.
Interviews with staff members and administrators showed a lack of training on codes and confusion on how to tell when a person was DNR or not.
In March 2018 at Collinsville Rehabilitation and Health Center, an employee was charged with neglect in the death of a resident when, according to charging documents, she failed to perform CPR on an 81-year-old woman in June 2017.
Patterson said low wages and a difficult job result in high staff turnover, making training and consistent care even more difficult.
“Staff turnover is huge and a terrible thing in this business. They might come to work for you for 9 bucks an hour, and down the road they can make 10 an hour so they drop you, you spent all that time and money on them and they leave,” Patterson said.
Ethics of the job
In January, a St. Paul’s staff member was charged with stealing identities of nursing home residents in order to buy himself furniture for his house. According to police, he accessed what should have been private information of residents for five years. In 2005, he had done the same thing in Swansea.
Eisele said based on what she saw at St. Paul’s, she was not surprised someone had easy access to confidential information.
“I can see how that would happen because sometimes in the nurse’s station there would be no one there, but the charts would be sitting right there,” she said.
Other policies put in place to prevent or catch elder abuse also do not always seem to be properly followed.
St. Paul’s received an L violation in November 2014 for not investigating reports of abuse, neglect or mistreatment of residents.
In 2014, multiple residents reportedly suffered serious injury at St. Paul’s, such as a resident who had multiple fractures after an unreported fall, another who had a black eye and a resident who woke up with a displaced fracture in her ankle.
According to CMS, the origin of the injuries was never resolved and they were not investigated by the home as possible elder abuse.
In 2017, Integrity Healthcare’s Smithton location was fined when CMS found the home’s administrator had no license to administer nursing home care in Illinois and had never been issued one. He had been working at the home for seven months.
Patterson said staff work best when they have a “mission in their heart” to care for other people, otherwise they may be missing that “person-centered care.”
“I always say, you have to realize we're getting people who are so fragile, we hold that fragility in our hands,” she said. “Are we going to cherish them or just say you're bed 1A? They're not that, they need to be who they are.”
Facilities can be a difficult environment, however, even for staff who have that person-centered care.
Some staff members say working at a home puts workers in morally difficult positions, forcing them to choose between keeping them jobs or reporting neglect.
In 2015, Premissa Acoff sued Autumn Meadows in Cahokia for wrongful termination when the home fired her for reporting neglect. The suit was settled in 2016.In 2017, she filed a suit against Lebanon Care Center for the same thing.
The suit against Lebanon Care Center alleges a resident was left to sit on a toilet “yelling for help” for an hour “due to inappropriate staff ratios in the facility.” According to her allegations, when Acoff reported the incident she was presented with a “job in jeopardy” write-up. She was fired the following week. The suit is ongoing.
Where's the money?
Families often spend thousands of dollars a month on nursing home care.
Pearson said even after her mother’s death, she wants answers about why she spent thousands of dollars a month for what she said was neglectful care.
“I would love to know where our $7,000 was going. Who's making all this money from this money I’m paying?” she said. “If you weren’t there every day, they’re not going to get the care they should be getting there, especially for $7,000 a month.”
According to St. Paul’s cost report, the facility spent about $7 million on total operating expenses in 2016.
While St. Paul’s home is listed as a nonprofit facility, many other homes in the area are part of larger, for-profit companies.
Many of metro-east’s nursing homes are corporate-owned. Some examples include:
▪ Helia Healthcare: operates Willowcreek and Four Fountains in Belleville and 12 total homes in Illinois and Missouri
▪ Peterson Healthcare: owns five Metro-east homes, including Lebanon and Swansea care centers, and nearly 100 nationwide.
▪ Integrity Healthcare: runs the 180-bed Midwest Respiratory center and 13 other locations.
▪ Bria Healthcare: owns two large nursing homes in the area in Belleville and Cahokia, along with 12 other Illinois locations.
▪ SW Management Co: operates Cahokia’s Autumn Meadows, Caseyville Rehab and five other homes
Buser called companies that own dozens of facilities across the state or the country “nursing home chains.” He said this vast network of facilities can cause a focus on profits instead of on proper care for residents.
Davis, whose company owns nursing homes, however, said while he understands why people may think this way, it is an “old perspective based on an old regulatory environment.”
“I disagree with the premise that owners are in it only for the profit,” he said. “I can tell you that margins may many years ago have been substantial, but they are now often times less than 1 percent, and many facilities are losing money.”
Comstock added some of these nursing home corporations have been handed down through families and many owners worked in the homes themselves at some point.
“Nursing homes take their responsibility for caring for residents and assisting families through this time very, very seriously,” she said.
How to find a home
For those trying to find a long-term care facility, CMS and IDPH offer online ratings of the homes and violation reports are available through CMS.
Patterson said it is just as important, however, to physically visit the home if possible to see if it is up to your standards.
“More than anything, I want people to realize that you have to be careful, you have to realize that places are operating in not a very good way,” she said.
Pearson said having her mom in St. Paul’s took an emotional toll on her entire family.
“We all had a lot of stress and anxiety,” she said. “It just makes us sick that she had to live out her last days like that.”
In May 2016, Waldron, 89, died at St. Paul’s Home.
Two years later, Pearson still has questions for the home about the care her mother received.
“We never got specific reasons on things. There were so many questions unanswered. We finally got to the point where it was exhausting trying to get answers.”
Davis and Comstock said they believe the majority of long-term facility care is positive, but people and the media are more inclined to focus on the negative.
“There are positive things happening in facilities every day, and those stories don’t get told,” Comstock said.
Davis said if things don’t change at the state level, like higher Medicaid reimbursements and timelier payments, resources for facilities will become even more limited.
“Unless some of those things change, we’re going to be left with even greater challenges,” he said.
This story was originally published May 14, 2018 at 1:43 PM with the headline "The metro-east has some of Illinois' worst nursing homes, data says. Here's why.."